The state of our state's coronavirus fight
We do not know enough.
How many will be infected? How many will die? Our best guesses are still only guesses, overshadowed by uncertainty.
How many have already been infected? Tens of thousands of tests have been run, but nowhere near enough to map the virus’ full spread.
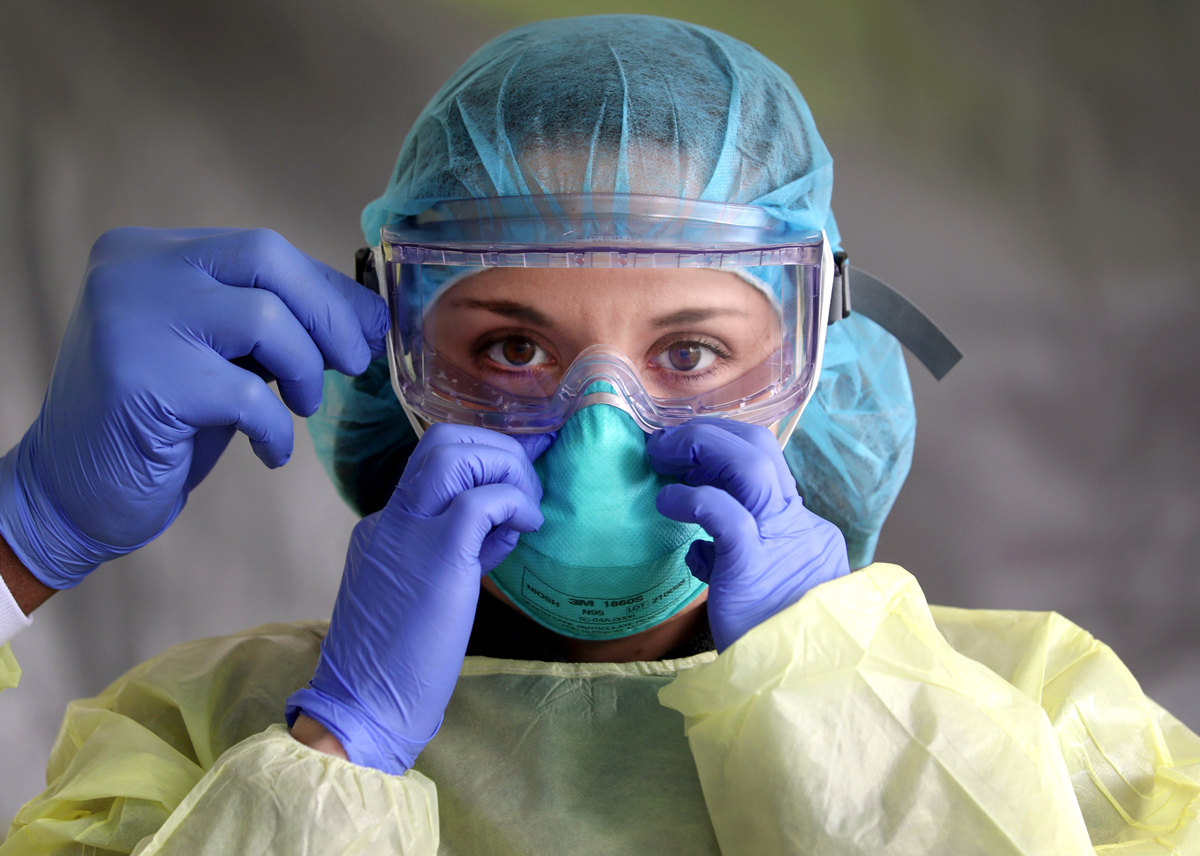
Do doctors and nurses have the protection they need? Not really, exposing them and their patients and families to dire risk.
Still, there is evidence for optimism. Our hospitals were going to be overrun. That danger seems to have passed. Those 500 ventilators the federal government sent us? Didn’t need 'em. The 250-bed emergency field hospital? The Army unpacked it one week and packed it up the next.
Send them to people who need them more.
The substantial sacrifices we all are making are saving lives.
But all around us, there remains an immense human tragedy.
In six weeks, nearly 500 people have died.
A taco truck owner, 44 years old. A married couple, 85 and 86, after 52 years of marriage, hours apart. A war veteran, refugee and father of nine, 72. A bus driver, 41. A corner grocer, the “heartbeat” of his neighborhood, 67.
All were loved. Almost none got to say goodbye.
Half a million people in Washington have lost their jobs. More will soon.
So much is uncertain, tenuous. If social distancing is working, what happens when we stop? When will we feel comfortable sending kids to school or going to restaurants or riding the bus or even passing someone on the sidewalk — let alone going to a crowded stadium?
When you’ve been told that every aspect of your daily routine has the potential to kill your loved ones, how do you go back?
As models increasingly show that Washington state is flattening the curve, The Seattle Times dispatched reporters to examine critical issues, from COVID-19 deaths to hospitalizations to supply chains for critical protective and testing equipment. The goal: to get a better sense of where we are now — what we know, and what we don’t.
— David Gutman
Predictions
Models forecast the epidemic’s toll, but they are highly uncertain

Mathematical models are one of the few tools available to forecast the spread of the new coronavirus and the impact of social distancing, especially since testing remains limited. Officials have relied on them heavily.
Early models, based on genetic analyses from Washington state’s first patients, suggested the pathogen had been spreading silently since mid-January. At the beginning of March, when the official count stood at 13 cases, scientists at the Institute for Disease Modeling (IDM) estimated there were probably more than 500 cases in Washington.
As the number of confirmed cases soared exponentially, IDM estimated that, if left unchecked, the virus could infect 25,000 people in King and Snohomish counties by early April, with 400 deaths likely.
The shocking numbers helped spur Gov. Jay Inslee to impose increasingly stringent measures to slow transmission. By late March, analysis of traffic patterns and anonymous Facebook data showed the measures seemed to be working. IDM scientists calculated that transmission rates had been roughly halved, which corresponds with a slowdown in the rate of new infections.
But modeling remains highly uncertain, based on assumptions about things that are still unknown, like the number of infected people with no symptoms and their role in spreading the disease.
Modeling from the University of Washington’s Institute for Health Metrics and Evaluation initially suggested Washington could see more than 1,400 deaths, even with social distancing, and warned hospitals could run out of beds.
But new data from Italy and Spain, where the epidemic seems to have peaked, led to major revisions last week. The group now forecasts about 842 deaths in Washington and says hospitalizations may have already peaked, with no bed shortages.
Looking forward, the models seem to agree on one point: If social distancing is rolled back too soon, infections and deaths will soar.
— Sandi Doughton
Read more about predictionsTesting
Testing access, plagued by problems, is improving
Widespread testing for COVID-19 in Washington remains spotty, plagued at times by limited availability of testing materials, laggard test results and persistent data problems.
The shortcomings point to an undercount of cases that blindfolds public health officials to the full extent of the virus’ spread.
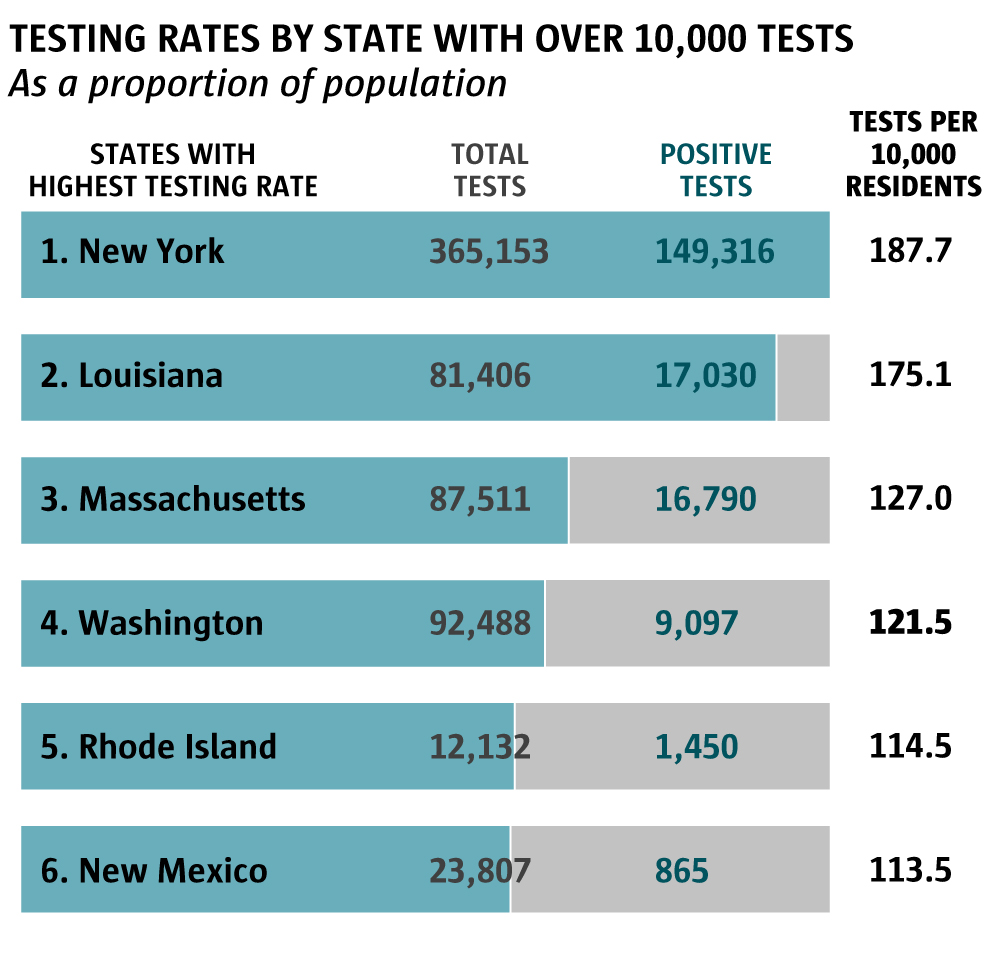
Sources: The COVID Tracking Project, U.S. Census (Emily M. Eng / The Seattle Times)
Nonetheless, Washington stacks up favorably when compared to other states.
Washington's nearly 122 tests for every 10,000 residents ranked only behind New York (188), Louisiana (175) and Massachusetts (127) among states that have performed at least 10,000 tests, based on the U.S. census and testing data monitored by The COVID Tracking Project. Overall, Washington was seventh nationwide in the total number of tests performed.
DOH has struggled for weeks to report timely, accurate data as it scrambled to fix a software problem in its infectious disease reporting system.
Washington’s troubles aren’t unique. Testing has been riddled with problems from the start, when the U.S. Centers for Disease Control and Prevention botched a nationwide rollout of test kits to public health labs.
Limited early testing allowed the virus to spread undetected in Washington, and problems persisted as the state tried to play catch-up. Testing availability, however, expanded statewide in recent weeks. As of Friday, at least 15 laboratories were operating, including several within some of the state’s biggest hospital systems.
Another glitch — slow turnaround times for test results — appears to be easing, as wait times up to two weeks or more in March have been dropping in April. UW Medicine’s virology lab, which handles most testing statewide, reports median test results of seven to 10 hours with expanding capacity.
One big problem remains: limited access to test kits, including swabs and specimen-preserving chemicals. Amid national shortages, UW Medicine went to great lengths to find suppliers in China and managed to ship 80,000 kits to Seattle last week, with the intention to buy more.
Widespread testing availability is “really fundamental to our ability to open up our community again and minimize the risk as we go forward,” said Jeff Duchin, health officer for Public Health - Seattle & King County.
— Lewis Kamb and Evan Bush
Read more about testingEquipment
Shortages of protective equipment hinder testing, leave health care workers exposed
Personal protective equipment (PPE) for frontline health workers — N-95 masks, gowns and face shields — that is necessary to safely test and care for COVID-19 patients remains in short supply in Washington.
But exactly how short is hard to say, as authorities don’t yet have a firm grasp on each health care facility’s inventory. Just a week ago, hospitals began reporting PPE levels to the Washington State Hospital Association (WSHA), which shares that data with state officials.
But as of midweek, the association’s president, Cassie Sauer, said some hospitals submitted incorrect information, and data gathering needed to improve. State officials did not respond to The Seattle Times’ request for information about statewide PPE inventory.
Because COVID-19 tests require more PPE than most diagnostic exams, the shortage hinders expansion of testing.

Until supplies are better stocked, hospitals and other facilities are reusing typically disposable equipment, following state guidelines. The Department of Health, for instance, recommends using N-95 respirator masks for eight hours, or disposing of them when visibly soiled or after certain types of patient contact. These conservation measures are helping strained supply levels hold steady, according to Puget Sound-area hospitals and health care systems.
UW Medicine hospitals, including Harborview Medical Center, had 114 patients admitted with COVID-19 symptoms as of Thursday morning and require caregivers to wear masks in all areas where patients are being treated. UW Medicine has an adequate amount of PPE because it's careful about what’s being used, spokesperson Susan Gregg said.
But many health care workers remain concerned. Some protested the lack of PPE outside hospitals around Washington on Thursday and called on the Trump administration to use the Defense Production Act to procure the gear.
State officials have been procuring PPE from private and public sources, including the Strategic National Stockpile. Since March 16, the state has acquired and distributed nearly 400,000 N-95 masks, a fraction of the 31.6 million it has ordered.
Meanwhile, health care administrators are getting creative. Some hospitals are recruiting community volunteers to sew masks. Sauer’s organization, which has no import/export experience, ordered 550,000 masks from China for smaller hospitals. She hopes Washington importers will step up to help during the pandemic.
“We have empty airplane capacity in this state,” Sauer said. “I would love it if somebody would get a plane to China and bring back a million masks.”
— Ryan Blethen and Mike Reicher
Read more about equipmentHospitalizations
Dire predictions of an overwhelmed hospital system have not come to pass
The forecast was ominous: “We anticipate that our hospitals will be in crisis by the end of the month,” wrote Gov. Jay Inslee in a March 17 letter to President Donald Trump requesting a Navy hospital ship drop anchor off Seattle.
More than three weeks later, the surge in hospitalizations has not emerged, thanks in part to social distancing measures and restrictions on elected surgeries.
Instead, Inslee recently sent ventilators and a military field hospital that never saw a patient back to the federal government for use in harder-hit states.
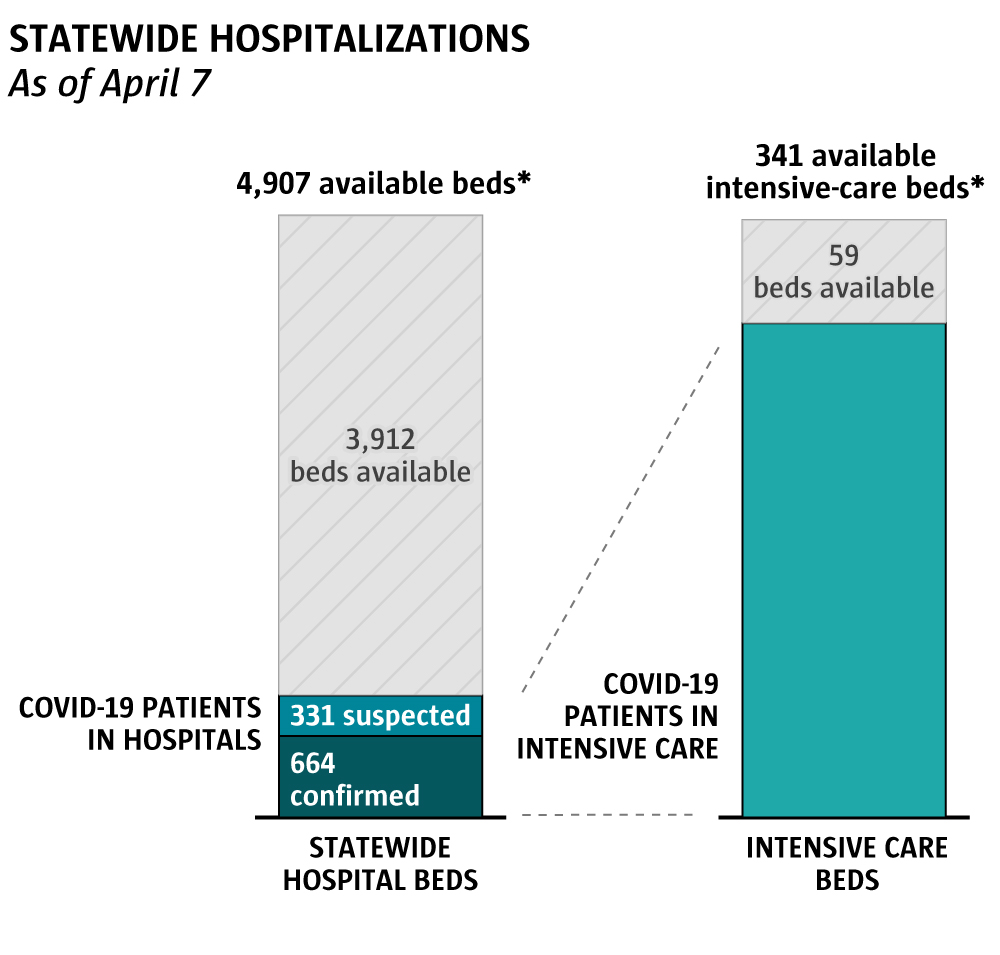
Sources: UW Institute of Health Metrics and Evaluation, Washington State Hospital Association (Emily M. Eng / The Seattle Times)
Through the spring, the state has had a spotty record in tracking hospitalizations, a key metric in the pandemic. State officials in March appeared to undercount the number of occupied beds. Last week, a new tracking system put in place April 2 began producing more accurate counts.
They indicated that there is substantial room for more COVID-19 patients that do not require intensive care. The margin of available ICU beds, however, is growing increasingly thin. But hospitals, large and small, are expanding the ability to care for these patients in part by delaying elective surgeries, an expansion not yet reflected in state hospital capacity numbers.
Hospitals still face a dilemma involving people who required surgeries during the epidemic — for a heart attack or a broken hip, for instance. Typically they would recuperate at a nursing home.
But those facilities — hit hard by pandemic — either stopped admitting patients or may have required multiple COVID-19 tests to prove they weren’t infected. As a result, hospitals have struggled to find beds for those patients to rehabilitate.
“We’ve so aggressively emptied out our hospitals,” said Sauer, with the state hospitals association. “But we are thinking we may be inadvertently overwhelmed, because people don’t have a place to discharge those folks.”
— Hal Bernton and Mike Reicher
Read more about hospitalizationsStaying home
How many of us are social distancing? It feels like a lot, but the data is imprecise
With restaurants and bars boarded up and schools shut down, Seattle certainly feels socially distant. But knowing exactly how many people are complying with government orders to stay home is an imprecise science.
Gov. Jay Inslee’s office focuses on the spread of the virus through rates of positive test results, hospitalizations and deaths, a spokesman said, but there are only imperfect measures to know how many of us are staying away from others.
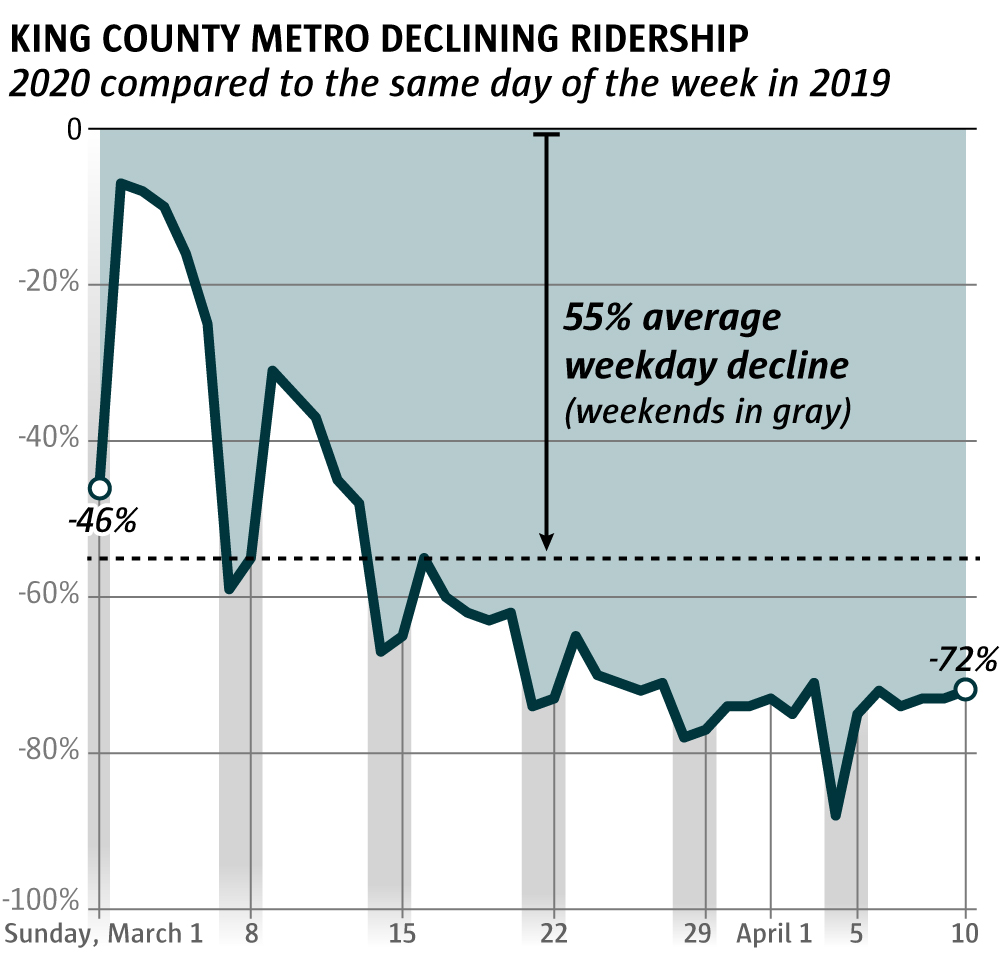
Traffic volumes on Interstate 5 through Seattle have fallen by at least half, and King County transit ridership has dropped 70 percent. Seattle police and automated cameras issued fewer traffic and parking tickets last month than in previous years, municipal court data shows.
But traffic drops have been more significant here than in some other parts of the state. And cellphone data showing how travel has reduced across the country also showed areas of southern and Central Washington where people appeared to be moving around more than the Seattle area.
Our garbage offers another clue. Overall solid waste volumes for Seattle Public Utilities have fallen 15%, with big drops in commercial areas, the city says. Water and electricity use are down, too, by between 2% and 6%, according to Puget Sound Energy, Seattle City Light and Seattle Public Utilities.
Other things are impossible to measure: how many people are passing too close to others on a sidewalk, sidling up in the grocery store checkout line or venturing on illicit Frisbee outings and clandestine visits to friends. Seattle police have been spotted in parks instructing groups of people to disperse.
One more count of who’s not staying home: Amid ongoing confusion over what exactly counts as “essential,” the state has received 13,000 complaints alleging nonessential businesses remain open, the governor’s office says.
— Heidi Groover
Read more about staying homeThe toll
Deaths continue to rise, but lower per capita than other hot spots

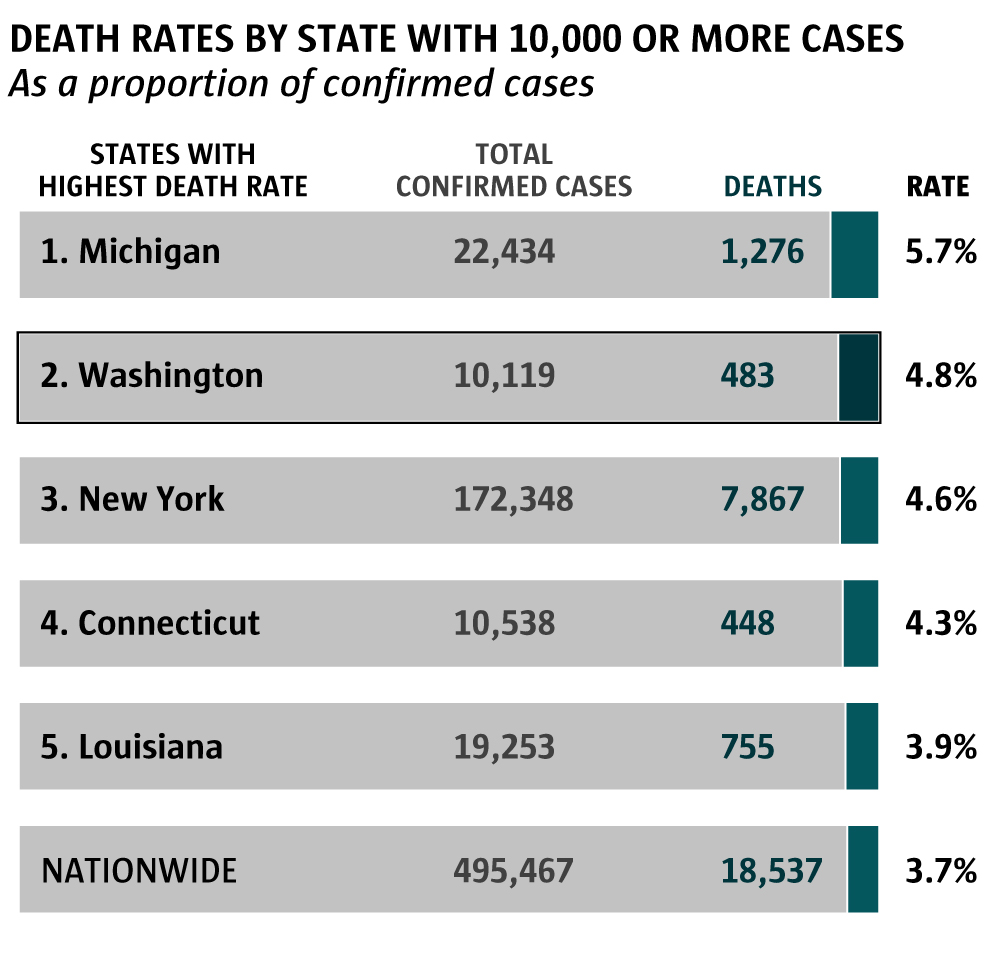
Source: Johns Hopkins University CSSE (Emily M. Eng / The Seattle Times)
Daily death totals from COVID-19 have climbed erratically — but climbed nonetheless — over the past two weeks, with more than 20 deaths a day reported nine days in a row through April 10.
When comparing Washington deaths to the number of confirmed cases, it’s a staggering death rate of nearly 4.8 percent of those infected, compared with 3.7 percent nationally and 4.6 percent in New York, the eye of the COVID-19 storm in the U.S. right now. For states with at least 10,000 confirmed cases, only Michigan had a higher death rate as of Friday at 5.7 percent.
Washington state DOH officials say those numbers are skewed by erratic and sluggish testing and other variables. Dr. Kathy Lofy, the state’s chief public health officer, believes a more accurate — if constantly shifting — view can be had using COVID-19 deaths per capita.
By that count, Washington’s COVID-19 death rate was 6.3 deaths for every 100,000 residents. New York was experiencing 40.4 deaths for every 100,000 residents; New Jersey and Louisiana — two other national hot spots — were seeing death rates of just over 21.8 and 16.2 deaths per 100,000 residents, respectively.
Using population figures and known deaths — while also likely an undercount — provides at least a view of where the virus is concentrated and promulgating, Lofy said. However, the real extent of the virus’s devastation won’t be known for months or years.
What is clear is that, in Washington, the death numbers were out of proportion early on due to the outbreak at the Life Care Center of Kirkland and a cascade of deaths among vulnerable residents at other nursing homes and care facilities. At least 200 of the state’s deaths were in senior care or group living facilities.
One number the state of Washington isn’t currently exploring: a count of people who have “recovered” from COVID-19, a figure kept by some other states and countries. Lofy said her investigators are too busy tracking new lines of infection to circle back on the more than 8,500 people who tested positive, got sick and didn’t die.
— Mike Carter
Read more about the tollEconomy
Unprecedented surge in joblessness follows economy into a deep freeze
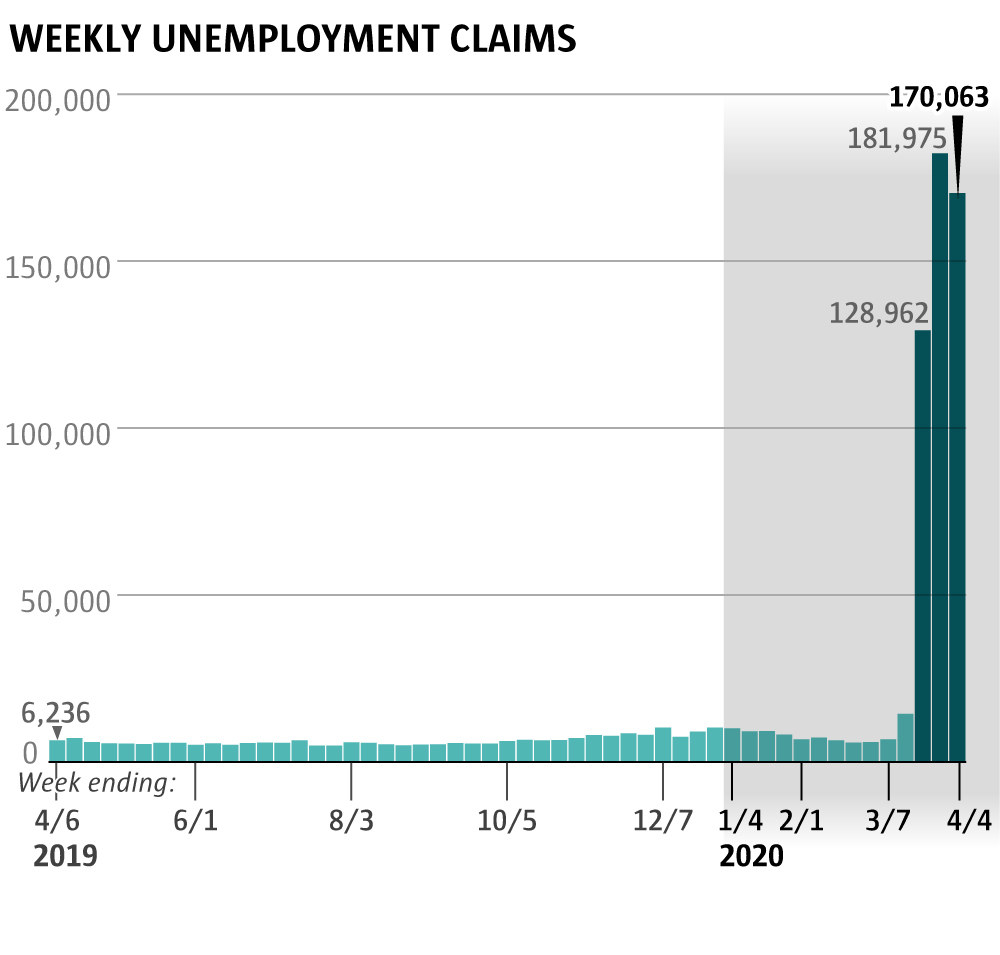
This past week's record-setting unemployment report underscores the deeper risk in the coronavirus crisis: that killing the virus will kill the economy.
As of last week, roughly one in eight state workers may now be out of a job. Thousands of businesses have closed — some permanently — and entire industries have shut down. In downtown Seattle, nearly two dozen hotels are closed, some reportedly at risk of default on their loans. And by some accounts, this is just the first wave.
The state Employment Security Department, already struggling under an unprecedented half-million unemployment claims, expects hundreds of thousands more in the coming weeks, as the paid leave offered by temporarily shuttered companies like Boeing and REI expires. Suzi LeVine, Employment Security Department boss, warns the state to brace for "a tsunami" of joblessness.
Already, food banks are seeing thousands of new customers. Applications for food assistance are up nearly 66%. And here, too, a second wave of damage is likely building, as families that barely covered April rent or mortgages are unable to do so on May 1.
As the damage mounts, there are growing fears of recession and rising political pressure to relax restrictions that show promise of containing the virus.
Even public health advocates understand that the longer the economy is shut down, the less likely the revival, and there is a real possibility that Gov. Jay Inslee’s stay-at-home order will extend beyond May 4.
Some of those anxieties may subside once federal aid starts to flow to reeling companies and laid-off workers. In theory, the damage is reversible.
But the fundamental problem remains: even with “enough cash getting to workers and enough cash getting to businesses,” economists are deeply fearful of fatally weakening the crucial links between workers and employees, said Brett Theodos, an expert in community development at the Urban Institute.
Even with massive federal stimulus, we may already be too late to avoid severe and possibly lasting damage, and not just to global players like Boeing. For small-business owners especially, the fear is they will survive the pandemic only to go bankrupt once it’s over.
Companies may also confront a permanently altered marketplace, with consumers more inclined to consume at home, and employees far more concerned about workplace safety and far less interested in coming to an office.
All this highlights the deeper challenge of bringing a post-industrial economy — and the community it supports — back from a pandemic.
Unlike the Great Recession, this recovery will require more than just trillions of dollars in federal stimulus. It will require a deep social and cultural and personal effort to restore the human relationships that make the economy possible.
— Paul Roberts
Read more about economy